Cupping therapy is commonly used in physical therapy to help reduce muscle tightness, improve mobility, and temporarily decrease pain sensitivity. During treatment, specialized cups create suction over restricted tissue areas, producing a gentle lifting effect across the soft tissue.
Many people seek dry cupping for neck tension, back pain, athletic recovery, stiffness, or movement limitations. At Calibration Physical Therapy in Overland Park, cupping is used alongside exercise, mobility work, and hands-on treatment as part of a broader rehabilitation plan.
What Does Cupping Do?
Cupping therapy creates negative pressure that lifts soft tissue instead of pressing into it. Physical therapists commonly use dry cupping to help address muscular tightness, improve tissue mobility, and make movement more comfortable.
Depending on the individual, cupping may help:
- Reduce muscle tightness and guarding
- Improve short-term range of motion
- Decrease pain sensitivity in irritated tissues
- Improve tolerance to stretching and movement
- Support recovery after exercise or repetitive activity
- Improve mobility in restricted soft tissue areas
Some patients describe the area feeling looser or less restricted after cupping. In physical therapy settings, that short-term reduction in stiffness or sensitivity may make it easier to stretch, exercise, or move through uncomfortable ranges of motion.
Cupping is not intended to “pull toxins” from the body or permanently fix movement problems on its own. In physical therapy, it is typically used as a supportive treatment alongside exercise, mobility work, and rehabilitation.
What Is Cupping Therapy?
Cupping therapy is a soft-tissue treatment technique that uses suction to gently lift tissue away from underlying structures. In physical therapy clinics, this is typically performed using dry cupping, a noninvasive method that does not involve incisions or blood removal.
Unlike massage, which applies downward pressure, cupping creates a lifting effect across the skin and superficial soft tissue. Physical therapists may use cupping to help improve tissue mobility, reduce muscular guarding, and make movement more comfortable during rehabilitation.
Dry Cupping vs. Wet Cupping
There are several forms of cupping therapy, but dry cupping is the method most commonly used in physical therapy and sports rehabilitation settings.

Dry Cupping
Dry cupping uses controlled suction to gently lift soft tissue without breaking the skin. Physical therapists may use dry cupping:
- Before mobility or stretching exercises
- Alongside manual therapy techniques
- To help reduce muscular tightness or sensitivity
- As part of post-exercise recovery treatment
Dry cupping is usually combined with other physical therapy treatments based on the patient’s condition and goals.
Wet Cupping
Wet cupping involves making small incisions in the skin before applying suction. This approach is associated with traditional and alternative medicine practices and is not performed in physical therapy clinics.
Because wet cupping involves blood removal, it carries different safety and hygiene considerations than dry cupping.
Benefits of Cupping Therapy
At a physical therapy clinic, cupping is typically used alongside exercise, mobility work, and manual therapy to help patients move more comfortably during rehabilitation.
Unlike massage, which applies downward compression, cupping creates negative pressure that gently lifts tissue. Physical therapists may use this decompressive effect to help improve tissue mobility and reduce sensitivity in restricted areas.
Potential benefits of cupping therapy may include:
- Reduced muscle tightness and stiffness
- Improved short-term mobility and range of motion
- Pain relief
- Improved tolerance to stretching and exercise
- Reduced feelings of restriction or guarding
- Support for athletic recovery and post-exercise soreness
Some patients report feeling looser or less restricted after treatment, particularly in the neck, shoulders, hips, or back.
A physical therapist may use cupping:
- Before mobility or stretching exercises
- Alongside manual therapy techniques
- During movement-based treatment
- To help reduce sensitivity in restricted areas
- As part of post-exercise recovery treatment
Results vary from person to person. Some patients notice relief after treatment, while others respond better when cupping is combined consistently with exercise and rehabilitation over time.
Rather than replacing active rehabilitation, cupping is used to help patients tolerate movement and exercise more comfortably.
Conditions Cupping May Help With
Cupping is commonly used in physical therapy for muscular tightness, movement restriction, and sensitivity in overworked or irritated tissues. It is typically combined with exercise, mobility work, and hands-on treatment rather than used as a standalone solution.
Physical therapists may use cupping as part of treatment for:
- Neck and upper trap tension
- Low back pain and stiffness
- Shoulder tightness and mobility restrictions
- Hip and glute tightness
- General muscular soreness and post-exercise stiffness
- Movement limitations related to soft-tissue restriction
- Sports recovery and repetitive-use irritation
- Tendinopathies, when combined with strengthening programs
For example, a physical therapist may use cupping before shoulder mobility exercises, alongside low back treatment, or after activity to help reduce muscular tightness and improve movement tolerance.
Treatment depends on the underlying condition, symptoms, activity level, and overall rehabilitation goals.
If muscle tightness, stiffness, or limited mobility is affecting your workouts, workday, or daily activities, our Overland Park physical therapists can evaluate whether dry cupping may be part of your treatment plan.
What Cupping Feels Like
Most people describe cupping as a gentle pulling or stretching sensation rather than pain. The intensity depends on the treatment area, amount of suction used, and overall tissue sensitivity.
After treatment, it is common to notice:
- Mild soreness similar to a workout
- Temporary skin discoloration
- Reduced feelings of tension or stiffness
- Temporary mobility improvements
Some patients describe the sensation as similar to a deep stretch or gentle pulling across tight muscles. Most people resume normal daily activity immediately after treatment.
Are Cupping Marks Bruises?
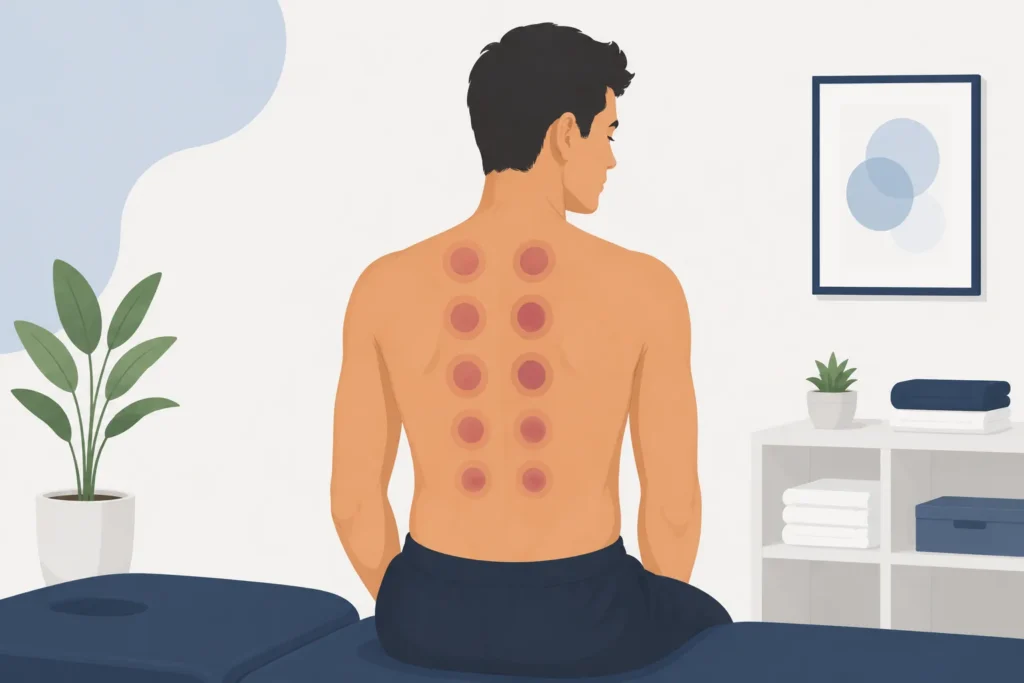
The circular marks left after cupping are one of the most common questions patients have about treatment.
Although the marks may resemble bruises, they are not considered bruises from blunt trauma. Instead, the discoloration is caused by temporary changes in blood flow and tissue response created by the suction.
Cupping marks:
- Are usually painless or only mildly tender
- Commonly range from light pink to dark red or purple
- Typically fade within several days to two weeks
- Vary depending on skin sensitivity and treatment intensity
Darker marks do not necessarily mean a worse injury or “more toxins.” In physical therapy settings, the marks are simply considered a normal tissue response to suction-based treatment.
At Calibration Physical Therapy, cupping intensity is adjusted based on patient comfort, skin response, and treatment goals.
Is Cupping Safe?
When performed by a licensed healthcare professional, dry cupping is generally considered safe for most people. In physical therapy settings, cupping is performed using controlled suction techniques designed to support movement and soft-tissue treatment.
The most common side effects are temporary and mild, including:
- Circular skin marks
- Mild soreness or tenderness
- Temporary skin sensitivity
- A feeling of tightness or warmth in the treated area
These effects typically resolve on their own within several days.
Dry cupping may not be appropriate for everyone. Physical therapists may avoid cupping over:
- Open wounds or active skin irritation
- Areas with infection
- Certain vascular or bleeding disorders
- Highly sensitive or fragile skin
- Specific medical conditions that increase bruising risk
Your physical therapist should review your medical history, medications, and treatment goals before beginning cupping therapy.
How Physical Therapists Use Cupping in a Treatment Plan
Physical therapists typically use cupping as one tool within a broader rehabilitation program rather than as a standalone treatment.
Depending on the condition being treated, cupping may be used:
- Before stretching or mobility work
- Alongside hands-on treatment techniques
- During movement-based treatment
- To help reduce sensitivity in tight or irritated areas
- After the activity to address soreness or stiffness
A session may involve stationary cups placed over restricted tissue or movement-based cupping, where patients gently move during treatment.
For example, a physical therapist might use cupping:
- Along the upper traps before neck mobility exercises
- Around the shoulder before range-of-motion work
- Along the hips or low back before strengthening exercises
- After activity to help address post-exercise soreness
Treatment is individualized based on symptoms, movement limitations, activity level, and overall rehabilitation goals.
In physical therapy settings, cupping is typically used to support movement and rehabilitation goals rather than as a passive, standalone treatment.
Cupping Therapy FAQs
What does cupping do?
Cupping therapy creates suction that gently lifts soft tissue rather than compressing it. In physical therapy settings, cupping is commonly used to help reduce muscle tightness, improve mobility, and temporarily decrease pain sensitivity.
What are the benefits of cupping?
Potential benefits of cupping therapy may include:
- Reduced muscle tension
- Improved short-term mobility
- Pain relief
- Improved tolerance to stretching and exercise
- Support for athletic recovery
- Reduced feelings of stiffness or restriction
Results vary depending on the condition being treated and the overall rehabilitation plan.
Are cupping marks bruises?
Cupping marks may look similar to bruises, but they are not caused by blunt trauma. The discoloration is a temporary skin and tissue response to suction created during treatment.
How long do cupping marks last?
Cupping marks commonly fade within several days to two weeks, depending on skin sensitivity, treatment intensity, and the area treated.
Is dry cupping safe?
When performed by a licensed healthcare professional, dry cupping is generally considered safe for most people. Mild soreness and temporary skin discoloration are the most common side effects.
Can cupping help with back or neck pain?
Physical therapists sometimes use cupping alongside exercise, mobility work, and manual therapy for neck tension, back pain, and muscular tightness. Treatment depends on the underlying condition and overall rehabilitation goals.
Can cupping help with muscle tightness?
Many people use cupping therapy to help address muscle tightness and movement restriction. Physical therapists often combine cupping with stretching, exercise, and manual therapy to help improve mobility and reduce tension.
Does cupping hurt?
Most people describe cupping as a pulling or stretching sensation rather than pain. The intensity can be adjusted based on comfort level and treatment goals.
Treatment recommendations vary depending on medical history, symptoms, and overall rehabilitation goals.
Final Thoughts on Cupping Therapy
Cupping therapy is commonly used in physical therapy to help address muscle tightness, movement restriction, and temporary pain sensitivity. While dry cupping is not used as a standalone solution, it may help some patients move more comfortably and tolerate rehabilitation more effectively.

At Calibration Physical Therapy, cupping is used alongside movement-based treatment approaches customized to each individual, rather than as an isolated, passive treatment.
Cupping Therapy in Overland Park
If tight muscles, stiffness, or movement limitations are affecting your workouts, job, or daily activities, our Overland Park physical therapists can evaluate whether dry cupping may be appropriate for your condition and goals.
Learn more about our:
Or contact our team to schedule a physical therapy evaluation.
Tags
About the Author
Dr. Traci Smiley, DPT
Traci is a licensed physical therapist and owner of Calibration Physical Therapy, serving the Kansas City area. A Board-Certified Orthopedic Clinical Specialist with advanced training in manual therapy and strength conditioning, she helps individuals overcome pain and return to what they love.





