A herniated disc is a common cause of back pain and leg symptoms such as numbness, tingling, or radiating pain. It is also a diagnosis that often sounds more alarming than it actually is.
In practice, a herniated disc is often very treatable. The key is understanding what it actually means, how symptoms typically behave, and how physical therapy helps people calm symptoms and return to normal movement.
What Is a Herniated Disc?
A herniated disc occurs when one of the discs in the spine becomes damaged, and some of its inner material protrudes through the outer layer. These discs sit between the vertebrae and act as shock absorbers for the spine during everyday movement.
You can think of a disc as a cushion that helps the spine tolerate bending, lifting, sitting, and twisting. When the outer layer weakens or tears, the inner material can push outward. Sometimes this causes only local back pain, while in other cases it irritates a nearby nerve.
Most herniated discs happen in the lower back. They can also occur in the neck, which may cause pain, tingling, or weakness in the shoulder, arm, or hand.
Where Herniated Discs Commonly Occur
Herniated discs can develop in different parts of the spine, but they are much more common in the lower back than in the mid-back. This reflects the load the lumbar spine experiences during everyday activities such as sitting, lifting, and bending.
In the clinic, lumbar disc issues are the most common PT sees. Cervical disc herniations are also common, but they usually show up with a different symptom pattern.
| Spine region | What patients often notice |
|---|---|
| Lower back (lumbar spine) | Neck pain with symptoms in the shoulder, arm, or hand |
| Neck (cervical spine) | Neck pain with symptoms into the shoulder, arm, or hand |
| Mid-back (thoracic spine) | Less common and usually more localized discomfort |
The location matters because it helps explain where symptoms are felt. A lower back disc problem may show up mostly as leg pain, while a neck disc problem may be felt more in the arm than in the neck itself.
What Causes a Herniated Disc?
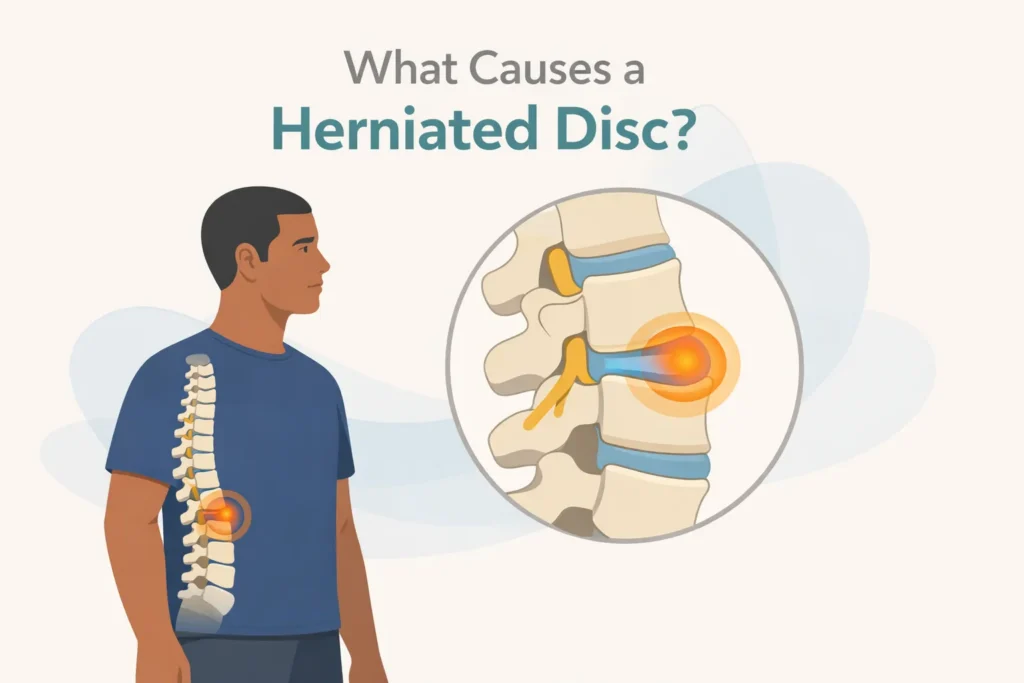
Most herniated discs do not occur out of nowhere. A lot of people associate them with one lift, one workout, or one awkward movement, but in many cases, the disc has been under repeated stress for a while before symptoms finally show up.
That stress can come from normal life. Repeated bending, long periods of sitting, deconditioning, and sudden spikes in activity can all make the spine less tolerant to load over time. Eventually, one movement or activity may trigger symptoms that bring the problem to attention.
Common contributors include:
- Repeated bending and lifting
- Prolonged sitting, especially when symptoms already flare with flexion
- A sudden jump in training, yard work, or other physical demands
- Reduced trunk and hip strength
- Normal age-related changes in the disc
That does not mean someone did something wrong. It usually means the spine was carrying a load it wasn’t ready to handle.
What Does a Herniated Disc Feel Like?

A herniated disc does not feel the same for everyone. Some people mainly feel pain in the lower back or neck. Others notice symptoms that travel, which often prompts them to wonder whether a nerve is involved.
When physical therapists hear someone describe pain traveling down the leg, symptoms that worsen with sitting, or tingling that changes with movement, that starts to build a clearer picture. The symptom pattern often matters more than the label itself.
Common symptoms may include:
- Pain in the lower back or neck
- Pain that travels into the buttock, leg, shoulder, or arm
- Numbness or tingling in the limb
- A sense of weakness or heaviness in the affected area
- More pain with prolonged sitting, bending, or lifting
A lumbar disc herniation may cause what people call sciatica, which usually means symptoms are traveling down the leg because a nearby nerve is being irritated. Sometimes the leg pain is actually more noticeable than the back pain, which can be surprising if someone expects the pain to stay only in the back.
How Symptoms Often Behave During Daily Activities
One of the most useful parts of evaluating a disc issue is looking at symptom behavior. Physical therapists are not just asking where it hurts. They are also trying to understand what makes symptoms ramp up, what settles them down, and whether the pain changes location during the day.
How symptoms respond to movement often provides more useful information than imaging alone.
| Activity | What patients often notice |
|---|---|
| Prolonged sitting | Back or leg symptoms increase, especially after staying in one position too long |
| Bending forward | Pulling, pain, or increased leg symptoms |
| Standing up after sitting | Initial stiffness or sharp discomfort before things loosen up |
| Walking | Sometimes improves symptoms, though longer walks can still irritate some cases |
| Lifting | Increased back pain or a feeling that the spine is not tolerating load well |
A common pattern is that symptoms worsen with flexed postures, such as slouched sitting or repeated bending, then improve somewhat with position changes or walking. While not every case follows this pattern, therapists frequently see it.
How Herniated Discs Affect Nerves
The reason disc herniations get so much attention is that they can irritate nearby nerves. When disc material protrudes, it can crowd the space around a nerve root or cause inflammation in that area. That is when people may start noticing pain, tingling, numbness, or weakness farther down the limb.
This is why a low back problem can cause calf pain, foot tingling, or symptoms in the buttocks and thighs. It is also why a neck disc issue can create pain or numbness in the arm or hand.
It is important not to panic when nerve symptoms are present. Nerve irritation does not automatically mean severe injury or permanent damage. Many people respond very well to conservative care, especially when symptoms are monitored early, and activity is adjusted appropriately.
How a Herniated Disc Is Evaluated in Physical Therapy

A physical therapy evaluation is not just a checklist of painful spots. The goal is to understand how your symptoms behave with movement, posture, loading, and position changes. That is what helps guide treatment.
Physical therapists focus on identifying movement patterns. Does sitting make things worse? Does walking help? Does bending forward increase leg pain? Does changing position reduce symptoms or bring them closer to the back instead of farther down the leg? Those details matter.
During an evaluation, a therapist may assess:
- Spinal movement in different directions
- Whether symptoms spread or reduce with repeated motions
- Strength, reflexes, and sensation when nerve involvement is suspected
- Hip mobility, trunk control, and movement habits during daily tasks
This is one reason imaging is only part of the story. Many people have disc bulges or degenerative changes on MRI without having meaningful pain. PT treatment is based on the full clinical picture, not just what shows up on a scan.
How Physical Therapy Helps a Herniated Disc
Physical therapy helps by reducing symptom irritability, improving movement tolerance, and gradually restoring the body’s ability to handle normal activity again. The goal is not just short-term pain relief. The goal is to help the spine tolerate everyday movement without repeatedly triggering symptoms.
Most disc injuries improve over time, but recovery often goes better when movement is guided rather than avoided. Physical therapy focuses on helping people move in ways that calm symptoms while gradually rebuilding strength and activity tolerance.
Treatment usually focuses on several key areas:
Reducing Symptom Irritability
Early in recovery, treatment often focuses on calming the irritated nerve and disc. This may involve adjusting positions, temporarily reducing certain activities, and identifying movements that help symptoms settle.
Examples of early strategies may include:
- Changing sitting posture or reducing long sitting periods
- Identifying movements that centralize symptoms back toward the spine
- Modifying lifting or bending patterns
- Using specific repeated movements that reduce nerve irritation
These changes are usually temporary. The goal is to settle the irritated tissues so normal movement can be reintroduced safely.
Restoring Normal Movement
When back pain begins, many people instinctively stop moving. While short rest periods can help initially, too little movement often leads to stiffness and increased sensitivity.
Physical therapy helps restore comfortable spinal motion and reduce fear around movement. As mobility improves, everyday activities like bending, reaching, and walking usually become easier again.
Improving Mobility Around the Spine
Sometimes the spine is not the only area contributing to symptoms. Limited mobility in the hips, mid-back, or surrounding tissues can increase stress on the lower back.
Improving mobility in these areas can reduce the load placed on the injured disc and make movement feel more natural.
Strengthening the Muscles That Support the Spine
The muscles around the trunk and hips play a major role in helping the spine tolerate everyday movement. When these muscles are weak or poorly coordinated, the spine may experience increased stress during activities such as lifting, running, or prolonged sitting.
Rehabilitation often focuses on strengthening:
- Core support muscles
- Hip stabilizers
- Glute and posterior chain muscles
- Muscles that help control spinal movement
Improving this support system helps the spine handle normal activity with less irritation.
Gradual Return to Activity
One of the most important parts of recovery is gradually returning to activity. Many people alternate between doing too little and doing too much, which can prolong symptoms.
Physical therapy helps guide a gradual return to activities such as:
- Walking and daily movement
- Gym exercise and strength training
- Running or athletic activity
- Work tasks that involve lifting or prolonged sitting
The focus is on building load tolerance over time so the spine becomes more resilient instead of more sensitive.
Who Often Benefits From Physical Therapy
Physical therapy is often helpful for people whose symptoms interfere with normal daily movement but do not require urgent medical care. Many patients seek care because pain keeps returning or because normal activities suddenly begin triggering symptoms.
In an outpatient orthopedic clinic, disc-related symptoms often appear in active adults who want to stay moving but are dealing with back or leg pain that keeps flaring up.
People who commonly benefit from physical therapy include:
- Runners who begin noticing leg symptoms during training
- People whose back pain increases during desk work or long drives
- Individuals who develop pain after lifting, yard work, or home projects
- Active adults dealing with recurring back stiffness that never fully settles
- Athletes trying to return to training without repeatedly triggering symptoms
For many of these patients, the goal is not simply to reduce pain. The goal is to help the spine tolerate normal activity again without constant flare-ups.
When Should You See a Physical Therapist?
Many episodes of back pain improve within a few days or weeks. However, certain symptom patterns make it helpful to have the problem evaluated sooner.
Pain that spreads away from the spine, keeps returning, or begins affecting normal movement is often a good reason to seek guidance.
You may want to schedule an evaluation if you notice:
- Back pain lasting more than a couple of weeks
- Pain traveling into the buttock, leg, or arm
- Numbness or tingling that keeps returning
- Weakness when walking, lifting, or using the affected limb
- Recurring episodes of back pain that seem easier to trigger each time
Early evaluation helps identify which movements irritate the spine and which are safe to continue. That often prevents the cycle of repeated flare-ups.
Final Thoughts
A herniated disc can sound intimidating, especially when it first appears on an MRI report. In reality, many people recover well with the right approach to movement and activity.
Physical therapy focuses on understanding how symptoms behave, improving spinal movement, and gradually rebuilding the body’s tolerance to everyday load.
If back pain or leg symptoms are limiting your movement, book an evaluation at our clinic to help identify what is driving the problem and create a plan that helps you return to normal activity safely and confidently.
Tags
About the Author
Dr. Traci Smiley, DPT
Traci is a licensed physical therapist and owner of Calibration Physical Therapy, serving the Kansas City area. A Board-Certified Orthopedic Clinical Specialist with advanced training in manual therapy and strength conditioning, she helps individuals overcome pain and return to what they love.





