Many people first hear about an MRI after visiting a doctor for joint pain, back pain, or an injury that is not improving. A provider may recommend imaging when symptoms have persisted for several weeks or when they want a clearer view of what may be happening inside a joint or soft-tissue structure.
MRI is one of the most detailed imaging tools used to evaluate muscles, tendons, ligaments, cartilage, and spinal discs. At the same time, imaging is only one part of understanding an orthopedic problem. This article explains what an MRI is, how it works, when it is used, and how physical therapy fits into treatment, even when imaging findings are present.
What Is an MRI?
MRI stands for Magnetic Resonance Imaging. It is a medical imaging test that creates highly detailed pictures of structures inside the body.
Unlike X-rays, which mainly show bones, MRI scans allow clinicians to see soft tissues clearly. These include muscles, tendons, ligaments, cartilage, spinal discs, and other connective tissues that often contribute to orthopedic pain.
MRI images are created as thin cross-sectional slices of the body. These slices allow clinicians to examine an area from multiple angles and better understand how different tissues relate to one another.
Because MRI captures soft tissue detail so well, it can reveal changes in tendons, ligaments, cartilage, and discs that may not appear on simpler imaging.
How an MRI Scan Works
An MRI scanner is a large machine that uses powerful magnets and radio waves to create detailed pictures of structures inside the body.
When a person lies in the machine, the magnetic field temporarily influences hydrogen atoms in the body. The scanner then sends radio waves into the area being examined. When those waves stop, the body releases signals that a computer converts into detailed images.
This process enables MRI to capture soft-tissue structures that are difficult to see on other imaging tests.
MRI is commonly used to visualize structures such as:
- Muscles
- Tendons
- Ligaments
- Cartilage
- Spinal discs
- Nerves
MRI does not use radiation. During the exam, the patient usually lies on a padded table that slides into the scanner, and most studies take between 20 and 45 minutes.
Patients are asked to remain still during the scan because movement can blur the images. The machine also makes loud tapping or knocking sounds, so ear protection or headphones are usually provided.
What MRI Scans Are Commonly Used For
MRI scans are most helpful when clinicians need detailed information about soft tissues. These tissues play a major role in how joints move and stabilize the body during activity.
When someone has persistent pain, weakness, or loss of function, an MRI can help providers understand whether structures such as tendons, ligaments, cartilage, or discs may be involved.
Orthopedic providers commonly order MRI scans to evaluate problems involving the:
- Rotator cuff tendons in the shoulder
- Knee ligaments, such as the ACL or MCL
- Meniscus cartilage in the knee
- Spinal discs in the neck or lower back
- Tendons around the hip, ankle, or elbow
- Joint cartilage that helps cushion movement
MRI may also help rule out more serious structural problems when symptoms include significant weakness, instability, or difficulty with normal daily activities.
Even when MRI findings are present, treatment decisions still depend heavily on how symptoms behave during movement and activity.
What an MRI Can and Cannot Show
MRI can reveal structural changes in muscles, tendons, ligaments, cartilage, and spinal discs. These images may show tissue irritation, swelling, tears, or degenerative change.
At the same time, imaging results do not always match how someone feels. It is common for MRI scans to show changes that are not actually responsible for a person’s pain.
This is especially true in the spine, shoulder, and knee. As people age, normal changes often appear on imaging even in the absence of pain or limitation.
For example, many adults who have never had back pain still show disc bulges on MRI. These findings often reflect age-related change rather than a true injury.
| MRI finding | What it may mean |
|---|---|
| Tendon irritation | Tissue may be overloaded or inflamed |
| Disc bulge | Common age-related change in the spine |
| Cartilage wear | Degenerative change in a joint |
| Minor ligament strain | Small tissue stress or stretching |
A helpful way to think about MRI is that it shows what the tissue looks like, but not always how the body is functioning. That is why imaging findings must be interpreted alongside symptoms, movement behavior, and activity tolerance.
What It Feels Like to Have an MRI
For most people, an MRI is a straightforward and painless test. The main challenge is usually remaining still while the images are being captured.
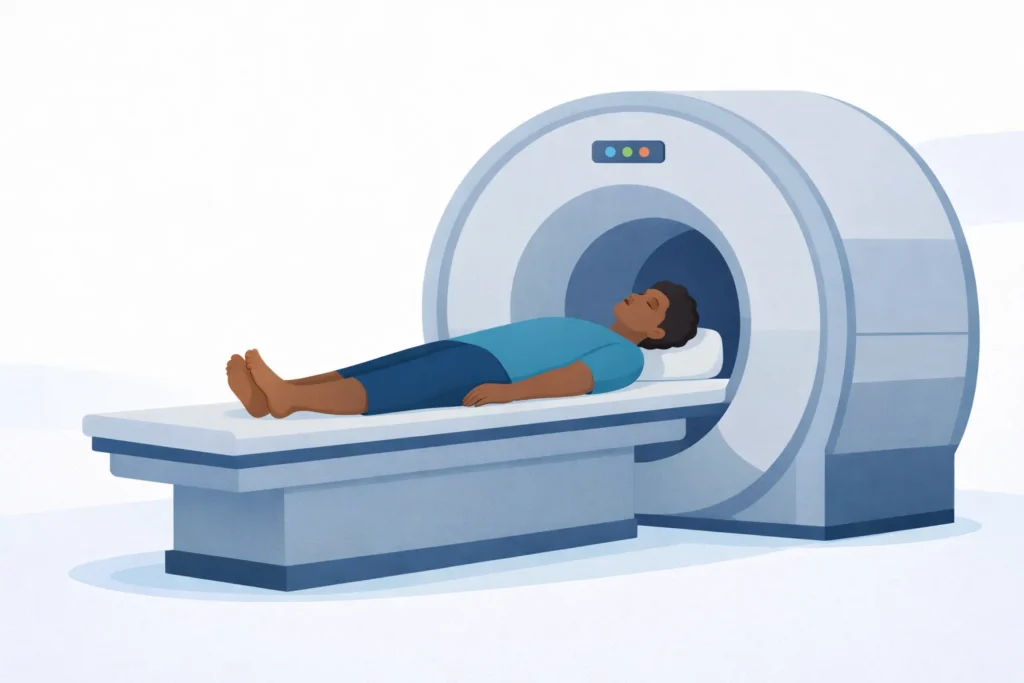
During the exam, the patient lies on a padded table that slides into the scanner. Depending on the body part being evaluated, the head, shoulder, knee, or spine may be positioned inside the center of the machine.
Some people feel a sense of tightness because MRI scanners are shaped like short tunnels. Imaging centers often help with this by offering music, headphones, or open MRI options.
Most MRI exams include a few simple steps:
- Lying on the scanning table
- Positioning the body part being tested
- Remaining still while images are taken
- Hearing the machine’s tapping sounds
In some cases, a provider may order an MRI with contrast dye to make certain tissues easier to evaluate. This is not required for many orthopedic MRI studies, but it is sometimes used when more detail is needed.
When Doctors Recommend an MRI
MRI is not usually the first step when someone develops joint or muscle pain.
Many orthopedic conditions improve with activity modification, physical therapy, or a short period of recovery. Because of this, clinicians often begin with a physical examination and conservative treatment before ordering advanced imaging.
An MRI may be recommended when symptoms persist or when providers need a clearer understanding of the structures involved.
Doctors may consider an MRI in situations such as:
- Pain lasting several weeks without improvement
- Symptoms interfering with normal daily activities
- Weakness or reduced joint stability
- Difficulty returning to sport or exercise
- Situations where surgery may need to be considered
The goal of ordering an MRI is not simply to get an image. It is to answer a clinical question, confirm a diagnosis, rule out more serious injury, or guide the next phase of treatment.
MRI vs X-ray: What Is the Difference?
X-rays and MRI scans are both imaging tools, but they serve different purposes.

X-rays are very effective for examining bones. They are commonly used to identify fractures, joint alignment problems, and signs of arthritis.
MRI scans provide detailed images of soft tissues, including tendons, ligaments, cartilage, muscles, and spinal discs.
Because many orthopedic problems involve soft tissues, an MRI may be recommended when symptoms persist despite normal X-rays.
| Imaging test | Best for showing |
|---|---|
| X-ray | Bones, fractures, joint alignment |
| MRI | Muscles, tendons, ligaments, discs |
| CT scan | Detailed bone structure |
In practice, clinicians often use imaging step by step. An X-ray may be performed first to rule out bone injury, and an MRI may be ordered later if soft-tissue injury is suspected.
Why MRI Findings Do Not Always Explain Pain
One important concept patients often learn during physical therapy is that structure and symptoms do not always match perfectly.
Someone may have clear MRI findings but very little pain. Another person may have significant discomfort even though imaging shows only minor structural changes.
This happens because pain is influenced by more than what appears on a scan. MRI shows tissue structure, but it does not measure how the body moves, how muscles coordinate, or how much load a joint can tolerate.
Pain is often affected by:
- Tissue irritation
- Movement patterns during activity
- Load placed on the joint over time
- Muscle strength and coordination
- Overall activity tolerance
For this reason, clinicians rely heavily on the physical examination and on how symptoms respond to movement and daily activity.
How Physical Therapy Evaluates the Problem
Physical therapists place a strong emphasis on how symptoms behave during movement and daily activity.
An MRI can show changes in tissue structure, but it cannot show how the body moves during real tasks. Because of this, a physical therapy evaluation focuses on movement patterns, load tolerance, and how symptoms respond to different positions.

During the evaluation, the therapist asks when symptoms occur and what activities make them better or worse. Pain during reaching, lifting, running, prolonged sitting, or sleeping positions often provides useful clues.
Movement testing often includes activities such as:
- Reaching overhead
- Squatting or bending
- Walking or running
- Lifting objects
- Rotating the trunk
Therapists also assess joint mobility, muscle strength, and how well different muscle groups work together during movement.
| Evaluation factor | What the therapist looks for |
|---|---|
| Movement patterns | How joints and muscles work together |
| Symptom triggers | Activities that increase discomfort |
| Range of motion | Whether joints move freely |
| Strength and control | Muscle support around the joint |
In many cases, this movement assessment provides more useful guidance for treatment than imaging alone.
How Physical Therapy Helps After an MRI
When MRI findings are present, treatment does not usually hinge on the scan results themselves. Instead, physical therapy focuses on improving how the body moves and how well tissues tolerate activity.
Rehabilitation often starts by reducing irritation in the affected area while maintaining comfortable movement. As symptoms improve, treatment shifts toward rebuilding strength, coordination, and activity tolerance.
Physical therapy may focus on:
- Improving joint mobility
- Restoring muscle coordination
- Increasing strength around the joint
- Improving tolerance to everyday activity
- Gradually returning to exercise or sport
These changes help the body distribute force more effectively during movement and reduce repeated stress on irritated tissues.
| Rehab phase | Focus of treatment |
|---|---|
| Early stage | Reduce irritation and restore comfortable motion |
| Middle stage | Build strength and movement control |
| Later stage | Increase activity tolerance and return to sport |
The goal is not simply to rest the area. It is to help the body regain the ability to handle walking, lifting, reaching, running, and other daily tasks without repeatedly aggravating symptoms.
Returning to Activity After Injury
Many people worry that MRI findings mean they need to completely stop exercising or avoid movement. In most cases, this is not necessary.
For many orthopedic conditions, recovery involves gradually improving the body’s tolerance to movement and load. Instead of avoiding activity altogether, physical therapy often helps patients modify their activity, so symptoms remain manageable as recovery continues.
Temporary adjustments may include:
- Reducing heavy lifting or high-impact activity
- Modifying running distance or intensity
- Limiting repetitive overhead movements
- Adjusting desk posture or sitting positions
- Gradually reintroducing challenging movements
As symptoms improve, activity levels are gradually increased. This graded return helps the body adapt safely and rebuild confidence in movement.
When to See a Physical Therapist
If pain, stiffness, or movement limitations are interfering with daily activities, a physical therapy evaluation can help identify potential contributors to the problem.
This is true whether imaging has been performed or not. MRI findings can provide useful information about tissue structure, but they do not always explain how symptoms behave during movement.
Physical therapists assess factors such as mobility, strength, coordination, movement patterns, and aggravating activities. These findings often reveal the mechanical reasons for the symptoms.
A physical therapy evaluation can help connect imaging findings with real-world function and create a plan for returning to activity.
Tags
About the Author
Dr. Traci Smiley, DPT
Traci is a licensed physical therapist and owner of Calibration Physical Therapy, serving the Kansas City metro area. A Board-Certified Orthopedic Clinical Specialist with advanced training in manual therapy and strength conditioning, she helps individuals overcome pain and get back to doing what they love.