Clicking in the jaw, facial pain, headaches, or difficulty chewing can all be signs of temporomandibular joint (TMJ) dysfunction. These problems can make everyday activities like eating, speaking, or even yawning uncomfortable.
The good news is that many TMJ problems respond very well to physical therapy. With the right combination of hands-on treatment, exercises, and posture correction, patients can often reduce pain and restore normal jaw movement without medication or surgery.
What Is TMJ?
The temporomandibular joint (TMJ) connects your lower jaw to the skull just in front of each ear. It allows the jaw to open, close, slide forward, and move side to side so you can talk, chew, yawn, and swallow.
Because the joint must move in multiple directions and coordinate with several muscles, it is more vulnerable to irritation and dysfunction than many other joints in the body.
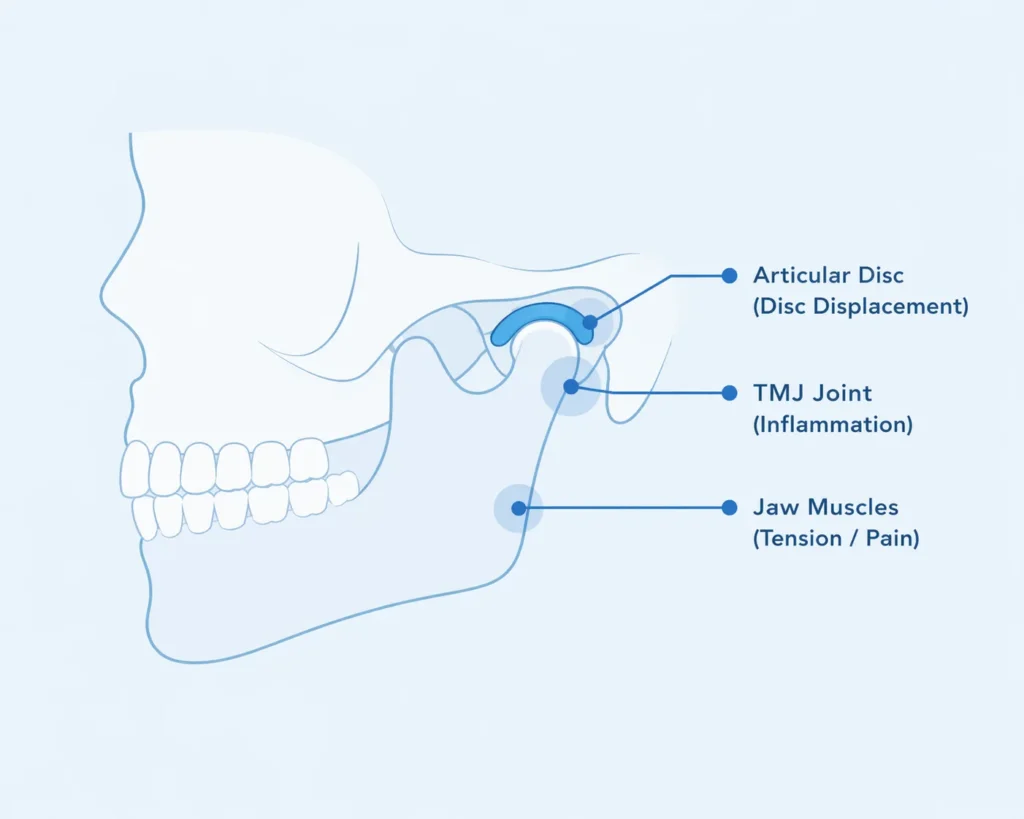
TMJ disorders (often referred to as temporomandibular disorders, or TMD) affect an estimated 11-12 million Americans. According to the National Institute of Dental and Craniofacial Research, women are diagnosed more frequently than men, and symptoms most commonly appear between ages 20 and 40.
TMJ dysfunction is commonly treated with physical therapy that focuses on reducing muscle tension, restoring jaw movement, and improving posture.
Recognizing TMJ Dysfunction: Common Signs and Symptoms
TMJ dysfunction can cause a wide range of symptoms. While jaw pain is the most obvious sign, many people experience problems in nearby areas such as the temples, ears, or neck.
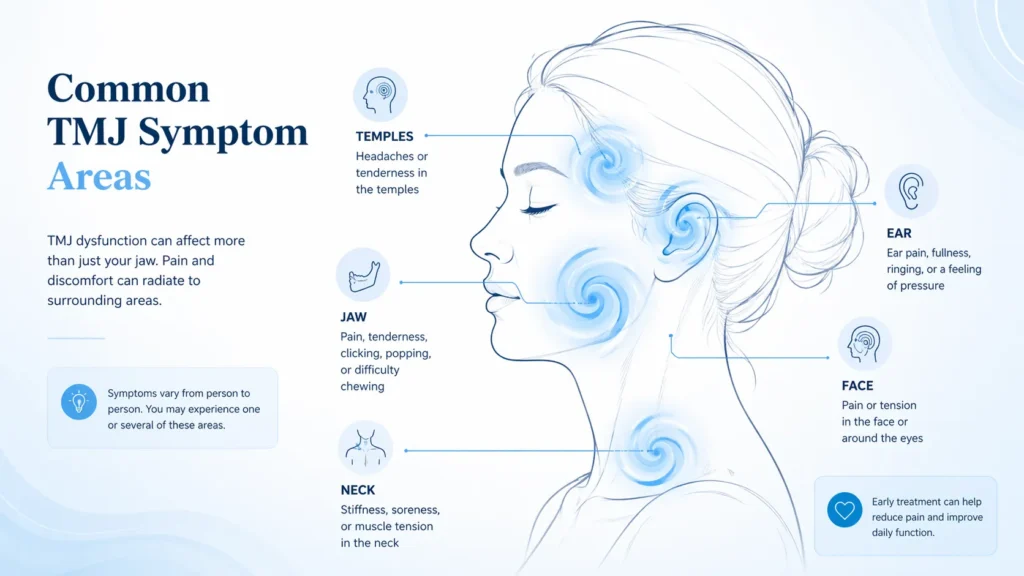
Common symptoms include:
| Symptom | What Patients Often Notice |
|---|---|
| Jaw pain | Pain near the ear, jaw joint, or along the side of the face |
| Clicking or popping | A noticeable sound when opening or closing the mouth |
| Difficulty chewing | Pain or fatigue while eating |
| Limited mouth opening | Feeling like the jaw will not open fully |
| Jaw locking | Jaw temporarily stuck open or closed |
| Headaches | Often felt in the temples |
| Ear symptoms | Ear pain, pressure, or ringing without infection |
| Neck tension | Stiffness or soreness along the upper neck |
While jaw pain is the most obvious symptom, many patients seek treatment for problems they never realized were related to their jaw.
Primary symptoms include:
- Pain or tenderness in the jaw, face, or around the ear
- Clicking, popping, or grating sounds when opening or closing the mouth
- Difficulty or discomfort while chewing
- A jaw that feels “stuck” or locks in position
- Difficulty opening the mouth fully
Related symptoms that often surprise patients:
- Headaches, especially in the temples
- Neck pain and stiffness
- Earaches or a feeling of fullness in the ears
- Tooth pain that doesn’t have a dental cause
- Dizziness
- Ringing in the ears (tinnitus)
If you’re experiencing several of these symptoms together, your jaw may be the missing piece of the puzzle.
What Causes TMJ Disorders?
TMJ dysfunction rarely has a single cause. More often, it develops from a combination of factors that stress the joint and surrounding muscles over time.

Muscle tension and overuse play a major role. Clenching your jaw during stress, grinding your teeth at night (bruxism), or habitually chewing gum can exhaust the muscles that control jaw movement. When these muscles become tight and fatigued, they pull the joint unevenly.
Posture also plays an important role in TMJ health. Forward head posture, which commonly develops from long hours at a computer or phone, changes the way the jaw sits relative to the neck and skull.
This position increases tension in the muscles that connect the jaw, head, and cervical spine. Over time, that added strain can contribute to TMJ irritation and jaw muscle fatigue.
Previous injury to the jaw, head, or neck can trigger TMJ problems, sometimes years after the initial trauma. Whiplash injuries are particularly associated with later TMJ dysfunction.
Arthritis can affect the TMJ just as it affects other joints, causing inflammation and changes to the joint surfaces.
Stress and anxiety contribute significantly to TMJ disorders. When we’re stressed, we tend to hold tension in our jaw and facial muscles, often without realizing it.
How Physical Therapy Treats TMJ: Our Approach
Physical therapy for TMJ focuses on reducing pain, restoring normal jaw movement, and addressing the underlying causes of dysfunction. Here’s what treatment typically involves.
Comprehensive Assessment
Your first visit includes a thorough evaluation of your jaw, head, neck, and posture. We’ll assess how your jaw moves, identify trigger points and areas of muscle tension, and look at how your upper body alignment might be contributing to your symptoms. We’ll also discuss your habits, stress levels, and daily activities that could be affecting your jaw.
Manual Therapy
Hands-on treatment is central to TMJ rehabilitation. Your physical therapist may use several techniques.
Soft tissue mobilization addresses the muscles inside and outside your mouth that control jaw movement. By releasing tension in the masseter, temporalis, and pterygoid muscles, we can often provide significant pain relief and improve jaw mobility.
Joint mobilization involves gentle, precise movements applied to the TMJ itself. These techniques help restore normal joint mechanics and reduce stiffness.
Myofascial release targets the connective tissue surrounding the jaw muscles and can relieve referred pain patterns that extend into the face, head, and neck.
Trigger point therapy targets specific muscle knots that can cause localized and referred pain.
Manual therapy and exercise-based approaches are supported by clinical guidelines for managing temporomandibular disorders, particularly when symptoms are musculoskeletal in origin.
Therapeutic Exercises
We’ll teach you exercises you can do at home to support your in-clinic treatment. These typically include:
- Jaw stretching and range of motion exercises that help restore normal movement patterns. These are gentle and controlled, never forcing the jaw beyond comfortable limits.
- Strengthening exercises for the muscles that stabilize and control the jaw. Like any joint, the TMJ benefits from balanced muscle strength.
- Postural exercises that address forward head position and rounded shoulders. Improving your overall posture takes stress off the jaw joint.
- Relaxation techniques that help you recognize and release jaw tension throughout the day.
Patient Education
Understanding your condition empowers you to manage it effectively. We’ll discuss:
- Dietary modifications during acute flare-ups (softer foods, smaller bites)
- Sleep positioning to reduce jaw strain
- Stress management strategies
- Habits to avoid, like nail biting, excessive gum chewing, or resting your chin on your hand
- Awareness techniques to catch yourself clenching during the day
What to Expect: Treatment Timeline
Many patients begin noticing improvement within the first few weeks of treatment. In general, meaningful progress often occurs within four to six weeks when therapy and home exercises are performed consistently. However, every case is different.
During your first few sessions, we focus on pain relief. Many patients notice reduced symptoms after just one or two visits as we address muscle tension and begin restoring normal movement.
Over the following weeks, we work on correcting movement patterns, building strength, and addressing contributing factors such as posture. This phase focuses on long-term improvement so the jaw moves comfortably and efficiently during everyday activities.
As you improve, visits become less frequent. We’ll ensure you have a home program that maintains your progress and helps prevent future flare-ups.
Some patients with long-standing or complex TMJ issues may need longer treatment. If your case involves structural problems within the joint itself, we may coordinate with your dentist or an oral surgeon to ensure you receive comprehensive care.
Why Physical Therapy Before Other Treatments?
When jaw pain develops, many people first visit their dentist or physician. That approach makes sense, but physical therapy is increasingly recognized as a first-line treatment for many TMJ disorders.
Because many TMJ problems are related to muscle tension, joint mechanics, and posture, conservative treatment often resolves symptoms without invasive procedures.
It’s conservative and non-invasive. Physical therapy doesn’t require medication, injections, or surgery. For many patients, hands-on treatment and exercises resolve the problem completely.
It addresses root causes. Rather than just managing symptoms, physical therapy corrects the muscle imbalances, movement dysfunction, and postural issues that contribute to TMJ problems.
It gives you tools for long-term management. The exercises and awareness techniques you learn in physical therapy stay with you, helping prevent recurrence.
Research supports physical therapy as an effective treatment for TMJ disorders. Systematic reviews and clinical guidelines consistently recommend conservative care, including physical therapy, as a first-line approach before considering invasive options.
This doesn’t mean physical therapy is the only answer. Some patients benefit from night guards, medication, or dental work, in addition to physical therapy. We’re happy to coordinate with your other healthcare providers to ensure you get the best possible outcome.
When to Seek Help
Don’t wait until your jaw pain becomes severe. Early treatment typically leads to faster, more complete recovery. Consider scheduling an evaluation if you experience:
- Jaw pain that persists for more than a few days
- Recurring clicking or popping in your jaw
- Difficulty opening your mouth fully
- Pain while chewing or talking
- Headaches that don’t respond to typical treatment
- Neck pain combined with any jaw symptoms
FAQs About TMJ Treatment and Physical Therapy
Do I need a referral to see a physical therapist for TMJ?
In Kansas, you can see a physical therapist directly without a physician referral. However, some insurance plans may require one for coverage. We’re happy to help you navigate your specific insurance requirements.
Will treatment be painful?
Some techniques, particularly those addressing trigger points or tight muscles inside the mouth, can cause temporary discomfort. However, we always work within your tolerance and communicate throughout treatment. Most patients find sessions relieving rather than painful.
How often will I need to come in?
Initially, most TMJ patients benefit from one to two visits per week. As you improve, we’ll space visits further apart. Your specific schedule depends on the severity of your condition and your response to treatment.
Can TMJ problems come back after treatment?
Yes, TMJ symptoms can return if contributing factors such as stress, teeth clenching, or poor posture are not addressed. That is why physical therapy focuses not only on relieving pain but also on improving movement patterns and teaching strategies to reduce jaw tension in daily life.
Maintaining good posture, avoiding excessive clenching, and continuing recommended exercises can help reduce the likelihood of future flare-ups.
Should I still see my dentist?
Absolutely. Physical therapists and dentists often work together on TMJ cases. Your dentist can address bite issues or provide a night guard if needed, while we focus on the muscular and movement components.
Finding TMJ Relief at Calibration Physical Therapy
Living with TMJ pain affects everything from enjoying a meal to having a conversation. You don’t have to accept it as normal.

At Calibration Physical Therapy, we take a thorough, hands-on approach to TMJ treatment. We’ll identify the factors driving your symptoms and create a personalized plan to restore comfortable, normal jaw movement. Schedule a TMJ evaluation today.
Tags
About the Author
Dr. Traci Smiley, DPT
Traci is a licensed physical therapist and owner of Calibration Physical Therapy, serving the Kansas City area. A Board-Certified Orthopedic Clinical Specialist with advanced training in manual therapy and strength conditioning, she helps individuals overcome pain and return to what they love.





